Klicken Sie auf Einstellungen, falls Sie diese ablehnen möchten.

Arterial hypertension is often silent, unnoticed, insidious and yet it affects vessels and organs throughout the body and increases the risk of heart attack and stroke up to ten times.
The Definition of Arterial Hypertension
Arterial hypertension, sometimes shortened to "hypertension" or "hypertonus", colloquially simply high blood pressure, is an abnormally high pressure in the arteries.
According to the WHO, this means a blood pressure of 140 systolic to 90 millimetres diastolic mercury column (mmHg for short) in practice measurements, 130/80 mmHg in 24-hour outpatient measurements and an average of 135/85 mmHg in home measurements. Systolic means the pressure in the vessels during the tension phase of the heart, when blood is pumped to the organs, and diastolic, when the heart muscle relaxes.
Although this is hardly noticeable, narrowing of the vessels (arteriosclerosis) and fatal heart disease can be the result. More than 20% of Central Europeans have high blood pressure, and only one in four people over 60 has normal blood pressure. Because the symptoms are often not noticeable at first, only a small proportion of those affected are treated in time.
Medicine distinguishes between primary (also essential) and secondary hypertension.
Secondary hypertension refers to an increase in blood pressure that is caused by another disease or an external influence, e.g. medication, hormone imbalances, hyperthyroidism, kidney problems, malformations of the aorta or drugs. Treatment of the causative disease is important in this case in order to lower the high blood pressure again.
For example, contraception with a hormone-containing preparation or hormone treatment during the menopause can influence blood pressure. Similarly, the menopause can promote high blood pressure because during this time a woman's oestrogen levels drop, which has a blood pressure-lowering effect.
Primary hypertension has no recognisable physical causes, is multifactorial and has not been conclusively scientifically clarified. However, its risk factors are known. If the primary hypertension is very difficult to control with medication, the presence of secondary hypertension must be considered. Sometimes primary hypertension can only be treated by reducing the risk factors.
The WHO also divides stages of hypertension according to the degree of damage: Hypertension grade 1 means hypertension without damage to the end organs. Hypertension grade 2 is used for mild damage and hypertension grade 3 for severe organ damage and secondary diseases.
High blood pressure is considered one of the four major risk factors for cardiovascular disease, along with diabetes mellitus, smoking and elevated cholesterol (hypercholesterolaemia).
The Symptoms and Consequences of High Blood Pressure
Arterial hypertension is often asymptomatic for a long time. The first symptoms may be a headache in the morning, insomnia, nausea, nosebleeds, fatigue, a red head, mental tensions and dizziness. In the course of time, shortness of breath, changes in the feeling of thirst and visual disturbances may occur.
Over time, high blood pressure hardens the blood vessels and promotes fatty deposits that impede blood circulation (constriction, arteriosclerosis). The list of possible consequences is then unfortunately long:
- renal insufficiency and failure (hypertensive nephropathy)
- heart attack
- stroke
- angina pectoris
- heart failure (or hypertensive heart disease HHK with heart failure)
- atrial fibrillation
- eye damage (hypertensive retinopathy)
- dementia
a.o.
Risk Factors for High Blood Pressure
Promoting risk factors are accordingly the same as for other heart diseases: Smoking, obesity, excessive alcohol and drug consumption, too much salt and unhealthy fat in the diet, too little exercise, nocturnal pauses in breathing, old age, heredity.
Psychosomatic factors have also been recognised for years as favouring factors, such as stress due to work situations, stressful family situations or anxiety.
Diagnosis and Therapy of Arterial Hypertension
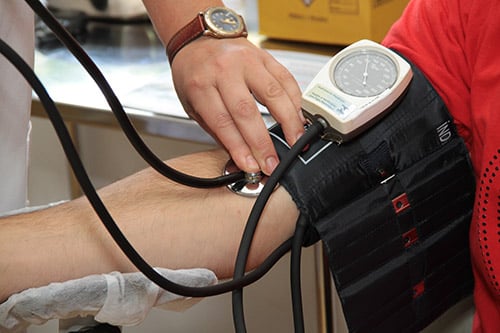
In order to diagnose arterial hypertension, blood pressure must be measured. 140/90 mmHg in a single measurement is not sufficient for a diagnosis. Only when elevated values are measured in at least three measurements within a few weeks can we be sure that there is elevated blood pressure. However, it is not always trivial to make the diagnosis, as some patients' blood pressure is only too high or fluctuates greatly under certain circumstances. In such situations, it is best to invest more time in clarification. An example of this is the so-called "practice or white coat hypertension". Some patients are nervous during a doctor's visit, which can manifest itself in short-term high blood pressure. In order to detect this temporary increase, patients can measure their blood pressure themselves at home or a long-term blood pressure measurement can be arranged.
The basis of the therapy is a change in lifestyle: heart-healthy diet, sufficient exercise, adequate sleep, weight reduction, smoking cessation, minimising the consumption of alcohol, sugar, salt, saturated fats and stress reduction.
Drug therapy is usually used for severely elevated blood pressure. There are many different active substances available, which are often combined with each other. If patients have side effects from the medication, it is almost always possible to find an active substance that is well tolerated.
One of the most common secondary diseases of untreated high blood pressure is heart failure or arteriosclerosis. This is when additional outpatient and inpatient therapies come into play to widen constricted vessels. (coronary angioplasty).
Below you will find an overview, recommendations and further reading on the subject of high blood pressure. Are you interested in an expert clarification of your symptoms or a cardiological check-up? We are happy to be at your disposal at our Heart Centre in Zurich.
Our link recommendations on the topic "Arterial hypertension (high blood pressure)"
Abstract "Arterial hypertension (high blood pressure)"
Arterial hypertension is a pathologically elevated pressure in the arteries. According to WHO, this means blood pressure readings of adults of 140/90 mmHg and above in practice measurements, 130/80 mmHg in 24-hour outpatient measurements and an average of 135/85 mmHg in home measurements.
- same as: high blood pressure, Hypertension, Hypertonus
- Organ: cardiovascular system
- Symtoms: shortness of breath (dyspnoea), weakness in performance, fatigue, asymptomatic, Headache, Dizziness, nausea, nosebleed, insomnia, visual disturbances, frequent urination
- Tests: ultrasound examination (echocardiography), blood pressure measurement, blood test, anamnesis, long-term blood pressure measurement
- Possible treatments: blutdrucksenkende Medikamente, weight reduction, sport activity, eating polyunsaturated instead of saturated or trans fats, smoking cessation, eat low salt, heart-healthy nutrition, alcohol reduction
- Risk factors: smoking, overweight, excessive alcohol consumption, too little exercise, stress, high age, heridity, diet too high in salt
- Possible differential diagnosis: varies depending on the symptom
The most important questions and answers about "Arterial hypertension (high blood pressure)"
How can you lower blood pressure?
Since high blood pressure can have many serious consequences, it is worthwhile to lower it. There are many "home remedies" available to you.
- Materials needed: Blood pressure monitor
- Required tools: pillbox, alarm clock or reminders, calorie and exercise counter
- Costs: 50 USD
- Time needed: 0.25 h
Steps
-

1 Lose Excess Weight
- Reduce your weight with a combination of long-term adapted, healthy and at the same time enjoyable nutrition and physical activity. Short-term diets often have the opposite effect. Take advantage of the support offered by nutritional counselling.
-

2 Planned Medication Intake
- Do not stop taking your medication when you are feeling better.
- Take medication regularly. Use pillboxes, placement in conspicuous places, combination with daily activities, alarm clocks, apps. Keep medicines in stock. Do not forget medication at home when travelling.
- Regularly discuss with your doctor which medicines you are taking and any side effects you observe.
-

3 Eat a Heart-Healthy Diet!
- Eat plenty of fresh vegetables, salads and fruits in all variations.
- Replace saturated fats with unsaturated fats: Replace sausages, fried foods and dairy products with olive oil, nuts, seeds and vegetarian or even vegan meals.
- Do not consume more than the WHO recommended amount of 5g of salt per day. Use dietary aids, as salt is in many different foods (e.g. in cheese).
- If you are dealing with heart failure, drink no more than 1.5 litres of fluid per day.
- Make sure you don't eat more calories than you consume each day. An app can help you learn and discover where the fatteners are hiding. Or which type of exercise burns how many calories. It's interesting and fun!
-

4 Move with the Right Moderation
- Walking and light hikes - with rest breaks.
- Cycling on home trainer or in nature.
- Exercise at the right time and adapted to your age and fitness: when you feel well, not after meals, at cooler hours. Stop if you experience shortness of breath or pain. Younger people can also do endurance and strength sports.
-

5 Reduce Stress
- Blue light from screens or LEDs reduces melatonin release. Use candles, salt stones and coloured lamps to simulate the light of a sunset. Your body will thank you.
- Try relaxation techniques such as yoga, meditation, walks, pets or talking to your loved ones.
- Get enough sleep.
- People with irregular daily routines are more likely to have sleep disorders, depression and heart attacks. Spare yourself by simplifying your life.
- Loneliness can be a stress factor and leads to a higher risk of heart disease. Enjoy the balance that social contact can bring.
-

6 Consume Stimulants with Caution
- Give up smoking. Use tools such as workshops, nicotine supplements and books to do so.
- Restrain yourself from alcohol and drink very little of it.
- Drinks containing caffeine, such as coffee, black tea, green tea, cola and energy drinks, but also dark chocolate can stimulate the heart and metabolism depending on habituation and increase blood pressure for 20-30 minutes (be careful when measuring). 400 milligrams per day is considered the recommended upper limit. Caffeine can increase cardiac arrhythmias. If you experience unwanted discomfort: Water helps to eliminate caffeine.